Skincare in Pregnancy is an important topic. Pregnancy heralds a big change in a woman’s life and also changes a woman’s body in many ways. Along with the gain in weight, some of the most noticeable changes are those in the skin, hair, and nails. Many of these changes can cause anxiety because they can affect the way you look. However, most of these ‘problems’ are harmless and will often go away after you give birth if you take proper skin care in pregnancy, because they are due to pregnancy-induced variations in your hormonal balance, metabolism and immune system.
Skin Problems in Pregnancy
These are mainly of three types –
- Common physiologic skin changes during pregnancy
- Skin diseases specific to pregnancy
- Pre-existing skin diseases and effect of pregnancy on them
Common physiologic skin changes in pregnancy
- Stretch marks (striae)
- Darkening of some areas of your skin
- Acne in pregnancy
- Changes in hair growth
- Spider veins and varicose veins
Stretch marks in pregnancy
Stretch marks (also called striae) are linear marks that most often develop over the breasts, abdomen, hips, and thighs.
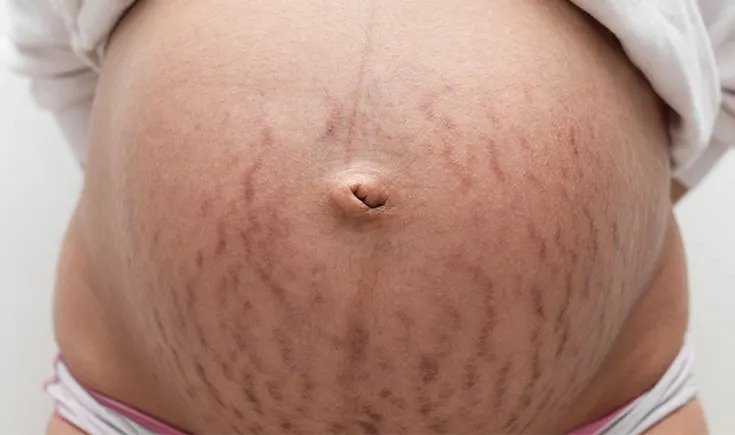
Stretch marks are caused by stretching of the skin beyond its elastic limit. They are very common in pregnancy, occurring in up to 50% to 90% of pregnant women. They begin as reddish purple lines and with time, they become white atrophic (wrinkled) scars. They are usually asymptomatic, but rarely may cause burning and itching.
They usually appear around the 25th week of pregnancy, although some women develop stretch marks even earlier.
There is no health risk to either mother or baby if stretch marks are present.
After delivery, stretch marks fade over a year or two, but do not disappear entirely.
Darkening of Skin
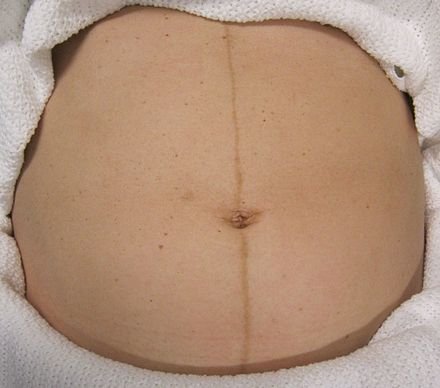
Dark patches on the cheeks and or forehead in pregnancy is called melasma or chloasma, also known as “the mask of pregnancy.” Other areas of skin which may darken include the nipples, genitalia, and Linea alba (line on your abdomen). In some women recent scars will darken.
If you notice any new or rapidly changing dark spots (or “moles”), show them to your doctor right away.
Melasma (Mask of Pregnancy)
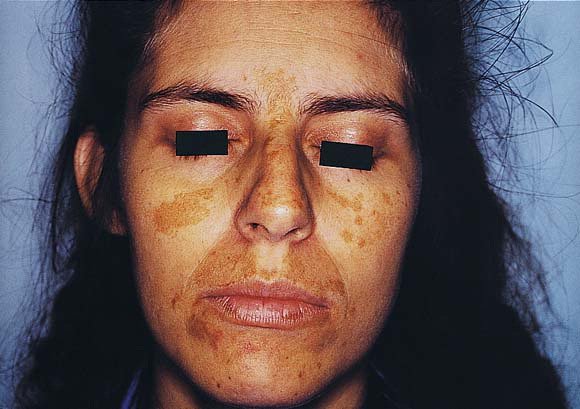
Facial pigmentation (melasma) is common in pregnancy and typically develops in the second trimester. Melasma worsens with sunlight exposure.
Skincare in pregnancy for melasma
The most effective strategy to prevent or help fade facial pigmentation is sun protection, including wearing a hat, staying in the shade, and the use of high sun protection factor (SPF 50) sunscreens.
Melasma may persist after pregnancy and a dermatologist consultation may be necessary.
Acne in pregnancy
Acne is primarily a result of increased hormone production in your pregnant body
Acne during pregnancy is very unpredictable Some women who have had a severe form of acne before becoming pregnant may find that their acne improves, and others who have never had acne may develop severe acne
Acne during pregnancy can be mild, moderate, or even severe, and it can occur at any time during the pregnancy. It may come and go, or it may last the entire pregnancy
Skincare in pregnancy for acne:
- • Avoid picking or scratching acne. It may worsen acne or cause scarring.
- • Wash gently with a mild soap or cleanser twice a day.
- • Don’t scrub your face with a washcloth, which can irritate the skin and make the problem worse. Instead, use your hands to gently wash your face.
- • Pat your skin dry rather than rubbing it.
- • If you use moisturizer, make sure it’s oilfree or non-comedogenic (which means they are less likely to cause acne).
- • Avoid irritants. Don’t use oily or greasy cosmetics, sunscreens, hairstyling products, or acne concealers. Use products labelled as water-based, mineral, or non-comedogenic.
- • Ask your dermatologist before using medicated gels or lotions. A number of over-the-counter and prescription products help improve acne, but some of the ingredients aren’t safe for pregnant women or haven’t been well-studied in pregnancy. If your acne is severe, you may need to see a dermatologist.
Changes in hair growth
During pregnancy, more hair goes into the resting phase (telogen) of the normal growth cycle of hair.
This causes diminished shedding of the hair, and it is perceived as thickening of the hair.
Three months after delivery, the hair cycle normalizes, temporarily causing increased hair loss in many women. This is called post-partum telogen effluvium. This process is usually completed six to twelve months after delivery.
After this, hair growth will return to normal. This temporary hair loss after delivery of a baby is normal and temporary
Pregnant women may experience hair growth in typical male sites, for example the beard area. This phenomenon is also related to hormonal changes (more male hormone, testosterone). Usually, it is not severe or permanent, and disappears within a couple of months of delivery
Spider Veins
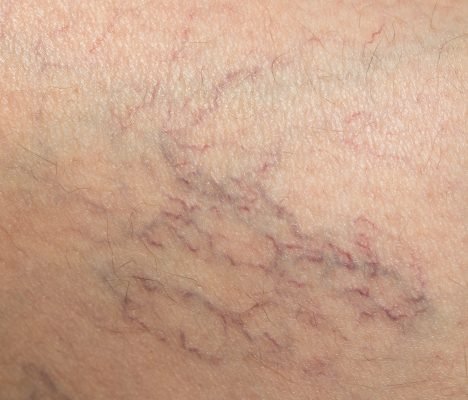
The increased amount of blood in your body during pregnancy can cause changes in your blood vessels. Tiny red, blue or purplish veins, known as spider veins, may appear on your skin.
Spider veins are most common during the first half of pregnancy. About two thirds of light-skinned pregnant women and about one third of dark-skinned pregnant women will have them on the face, neck, and arms. The redness should fade after giving birth.
Varicose Veins
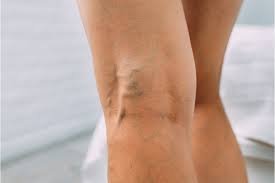
The weight and pressure of your uterus can slow blood flow from your lower body and cause the veins in your legs to become swollen, sore, and blue. These are called varicose veins. They also can appear near your vagina and rectum (usually called hemorrhoids). In most cases, varicose veins are not a problem. You are more likely to have varicose veins if someone else in your family has had them.
Skincare in pregnancy for varicose veins
Although you cannot prevent them, there are some things that can help the swelling and soreness and keep varicose veins from getting worse:
- If you must sit or stand for long periods, be sure to move around from time to time.
- Do not sit with your legs crossed.
- Prop up your legs—on your desk, a couch, a chair, or a footstool—as often as you can.
- Exercise regularly—walk, swim, or ride an exercise bike.
- Wear support hose.
Skin Diseases specific to pregnancy
Certain skin conditions can arise during pregnancy. They can cause discomfort, which often can be relieved with treatment.
Polymorphic Eruption of pregnancy
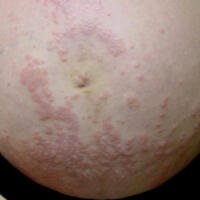
Polymorphic eruption of pregnancy starts in late pregnancy as small, red bumps and hives . The bumps can form large patches that can be very itchy. It often starts on the abdomen and can spread to the thighs, buttocks, and breasts.
The rash disappears after delivery
Your doctor may prescribe an anti-itch cream or steroid cream to help stop the itching.
Atopic eruption of Pregnancy
AEP includes women who already have eczema but experience a flare-up of the disease
Some patients present with atopic skin changes for the first time during pregnancy, but they often have a history of sensitive skin with a tendency toward dryness and irritation and often have first-degree relatives with eczema, asthma, and/or hay fever.
AEP usually develops during the first half of pregnancy (75% before the third trimester
The rash is very itchy and can be bad enough to interfere with sleeping. The severity of the rash depends on the type of AEP. If you suffer from worsening of preexisting eczema, it is likely that your skin will be red and dry. When the eczema is very active (during a “flare-up”), you may develop small water blisters on the hands and feet, or your skin may become wet and weepy. In areas that are repeatedly scratched, the skin may thicken in response – a process known as lichenification.
AEP can last for several months, and may even continue a while after the baby is born. It is usually treated with medications.
Pemphigoid Gestationis
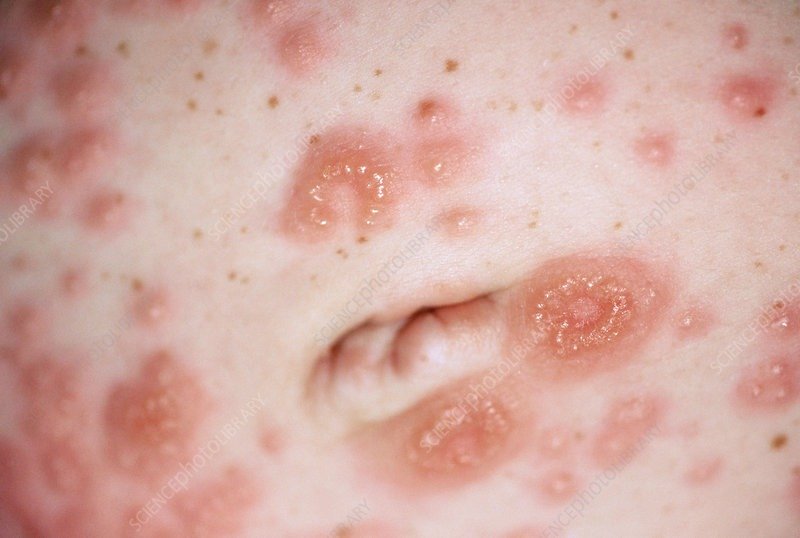
Pemphigoid Gestationis is a rare skin condition that usually starts during the second and third trimesters or sometimes right after a woman gives birth.
Pemphigoid Gestationis is an auto-immune blistering disease which means that the woman’s immune system reacts against her own skin causing skin blistering. Female hormones (particularly oestrogen) are thought to aggravate the reaction, and this may be why it starts during pregnancy when oestrogen levels rise
With this condition, blisters appear on the abdomen, and in severe cases, the blisters can cover a wide area of the body. Sometimes the condition returns during future pregnancies.
If your doctor diagnoses pemphigoid gestationis after checking your blisters, you and your baby will be monitored closely during the last part of pregnancy. Your doctor also may give you medications to control the outbreak of blisters and help relieve your discomfort.
Cholestasis of Pregnancy
Cholestasis is the most common liver condition that occurs only during pregnancy. It is caused by a defect in the excretion of bile from the liver resulting in rising bile acids in the blood.
The main symptom is severe itching on the palms of the hands and soles of the feet that later spreads to the rest of the body.
Symptoms usually start during the third trimester but often go away a few days after delivery. Cholestasis can come back, however, in future pregnancies.
If your doctor diagnoses the condition after taking blood tests, you and your baby will be monitored closely during the third trimester. This is because cholestasis may increase the risk of preterm birth and other problems, including fetal death.
Your doctor also may suggest using anti-itch creams and other medications to help relieve the itching and discomfort.
Preexisting Skin Conditions and Pregnancy
Women with certain skin diseases before pregnancy may see their conditions worsen or improve while they are pregnant. f you have any type of skin disease, let your doctor know if you notice any changes in your symptoms while you are pregnant.
Skincare in Pregnancy: Key Points
- Use mild non-perfumed soaps or cleansers
- Moisturize your skin regularly and especially after bath
- Use a sunscreen when outdoors
- Do not use medications without consulting your doctor. Some acne medications like retinoids and bleaching creams like hydroquinone are contraindicated in pregnancy

Also read Safe Skin care Guide in Pregnancy.
Finally…
The changes that happen to your skin, hair, and nails when you are pregnant can be bothersome. Luckily, most of them will go away once you give birth. In the meantime, with your doctor’s help, there are many ways to help you cope with the discomfort.

